Patient Times for Convenient Care
The provider's guide to the patient's mind.
Featured Article
Top articles
What's new

Urgent Care Excellence—Where Culture, Operations, and Finance Meet
Amid a challenging economic climate and widespread healthcare staffing shortages, many urgent...

Winter Wait Times: Balancing Patient & Staff Experience
With flu and respiratory illnesses running rampant, winter can be a wildly busy time for urgent...

7 Frequent Front Desk Mistakes and Effective Solutions
A seamless front desk process isn't just a convenience; it's a core patient expectation and a...

Urgent Care Patient Journey: A Roadmap to Improved Patient Throughput
As respiratory and flu season ramps up, many urgent care clinics find themselves stretched thin....
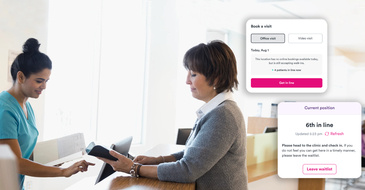
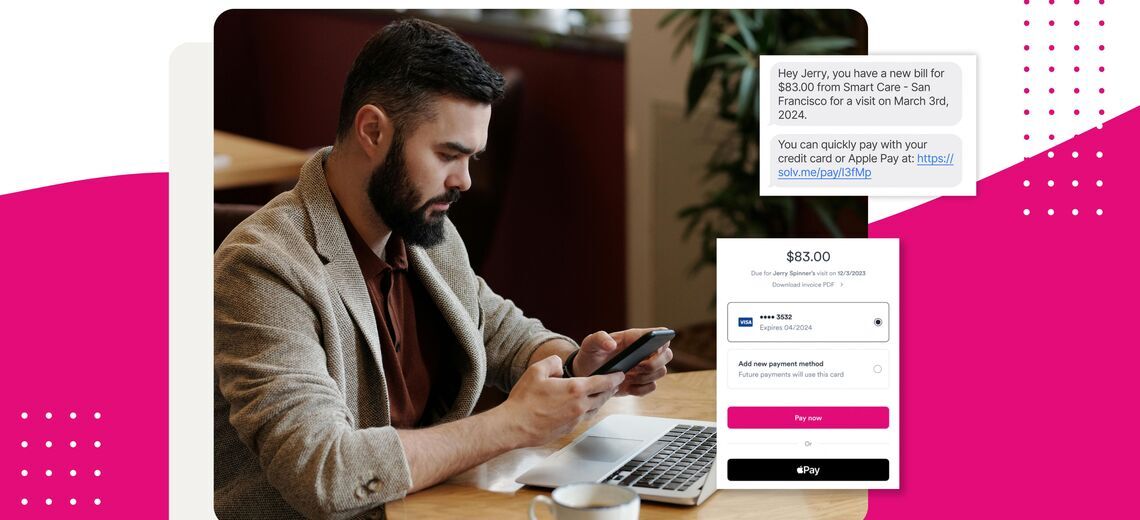
Product Spotlight: Capture More Patients and Allow Them to Wait Rem...
As we wade into another busy respiratory season, patient volumes will be unpredictable. Clinics...

The Operator’s Guide To Reduce No Show Patients in 2023
In the U.S., no-show rates average around 18.8% between specialty and subspecialty clinics. If...

The Impact of Leadership on Front Desk Performance
The front desk plays a crucial role in any urgent care, holding the key to improving patient...

Claim Submission Optimization: Faster Payments, Fewer Errors
For urgent care organizations looking to ensure prompt payment and a healthy revenue cycle,...

5 Common Patient Experience Mistakes
A positive patient experience is the foundation for improved patient relationships, higher...

Mastering the Art of Responding to Neutral 3-Star Reviews
In the world of online reviews, we often focus on the extremes: the glowing 5-stars and the...

Data-Driven Expansion: Leveraging Patient Behavior for Health Syste...
As a part of our series Sip & Strategize: Exploring Health Systems Business Strategy, in this...

How to Hire and Interview Front Desk Staff for Urgent Care
Often the first touchpoint for patients at urgent care clinics is the front desk staff. Front...
![How seamless is your patient intake process? [Quiz included]](https://d1kve3ll6vvkpr.cloudfront.net/dir/media/W1siZiIsIjIwMjMvMDcvMjEvMTcvMTQvNDcvYzcyYzdhNjYtNGY3Mi00MzhkLWIwYWYtYzkzYzg1ZTNmMzMzL2hvc3BpdGFsLWc3YWE2NzI5N2VfMTI4MC5qcGciXSxbInAiLCJ0aHVtYiIsIjM2NXgxOTAjIl0sWyJwIiwiZW5jb2RlIiwianBnIiwiLXF1YWxpdHkgOTUiXV0/file.jpg?basename=How+seamless+is+your+patient+intake+process%3F+%5BQuiz+included%5D&sha=e22919b3e946498e)
How seamless is your patient intake process? [Quiz included]
Take our self-evaluation quiz to discover how seamless your patient intake process is, and...

Metrics to Track for Improved UC Experience Performance
Urgent care facilities have seen a rapid rise in demand over the past few years. According to the...

Urgent Care & Health Systems: Fee for service and value-based care ...
About 15 years ago, a health systems strategy for financial success typically involved optimizing...

4 Business Outcomes of Patient Self-Scheduling
Having access to care has always mattered, but the speed to which you can access care has...

Best Practices Guide: Meet Patient Expectations and Grow your Busin...
Discover patient insights to inform your operations and book of business, and use that to...

Why Urgent Care Centers are Valuable to Health Systems in 2023
You've likely heard the question: Is this ER-worthy, or should I just head to urgent care? In...

Are Your Claim Rejections Soaring? Accurate Registration Tools Can...
You’ve streamlined everything in your urgent care business–optimized your marketing, integrated...

The Price of Unchecked Tech Debt
Frontline healthcare workers and healthcare technology professionals saw the critical impact of...

Robotic Process Automation: Save Time and Increase Accuracy
How long does it take to manually enter a new patient’s information into your electronic health...

Holiday Season Checklist: 4 Ways to Prep Your Urgent Care for the B...
As the end of the year approaches, it seems like calendar pages are flying off like a time-lapse...

5 Things Urgent Care Can Learn From Starbucks
The Urgent Care Association recently tweeted that there are more urgent care centers than...

4 Key Ways to Prepare Operations Before Respiratory Season
One of my favorite parts of my job is visiting our Solv partners and getting a first-hand look at...

4 Ways to Fight Inflation in Urgent Care
If COVID was the villain of 2020 and 2021, it’s being upstaged by a more subtle but still...

The Complete Guide to Urgent Care Financial Management
Financial health and profitability are perpetually top of mind for urgent care executives,...

6 Things Urgent Care Brands Can Learn From Apple
In the late 90’s and early 2000’s, Apple transformed the already-booming technology industry with...

Seven Tasks Every Urgent Care Should Automate
On any given day, an urgent care can see hundreds of patients–the ins and outs of high acuity...

Increase Clinic Revenue by Avoiding Acuity Degradation
Imagine this–a child falls on the playground and seems to have fractured an ankle. Where would...

5 Things We Learned From Scheduling 22 Million Urgent Care Visits
Your book ahead and walk-in patient volumes have probably decreased this last few weeks. How are...

5 Ways Telemedicine Services Streamline Urgent Care Operations
The pandemic revolutionized the face of modern medical care. New vaccine technology was utilized,...

5 Important Lessons Healthcare Providers Can Learn From 2021
2021 was a roller coaster of a year for healthcare providers. After a tough year, we thought...

5 Secrets to Retaining Your Medical Office Front Desk Staff
In 2018, Mercer predicted that demand for healthcare workers will outpace supply by 2025...

5 Tips to Improve The Front Desk Workflow At Your Medical Office
You understand that your front desk staff isn’t just answering phones and letting the doctor know...

4 Ways To Revolutionize Your ED Diversion Strategy
Emergency department (ED) diversion is a long-standing strategy that is deployed when hospital...

We’re Open: Renewing Our Commitment to Interoperability with New EH...
Solv’s new EHR integrations and automations eliminates work for the front desk and improves data...

5 Strategies to Effectively Manage a Surge of Patients This Holiday...
*this blog was originally published on 11/19/2020 and has been updated for clarity. As traffic...

Does your EHR pass the interoperability test?
Solv’s new Robotic Automation technology opens up closed EHRs and unlocks opportunities for...
The Changes that Healthcare Operators Need to Make Coming into This...
“It was the best of times, it was the worst of times...it was the season of light, it was the...

6 tips for optimizing community-based COVID-19 testing
Recent data from the Covid Tracking Project report a national daily average of 802,000 tests,...

Hybrid Care: How to Effectively Incorporate Telemedicine into Your ...
Solv is committed to providing the primary care industry with easy-to-use solutions that will...

Contactless Clinic Experiences and a New Way Forward
Cafes. Libraries. Retail centers. The Taco Bell down the street, the locally-owned liquor store...

Consumer behavior is driving a hybrid approach to healthcare delivery
As states begin reopening and social and medical distancing restrictions are relaxed, the...

Telemedicine Reimbursement: A Guide to Payment Parity and Covered S...
Every day, as new developments around COVID-19’s impact continue to be discovered, policymakers...

COVID-19 and the Rise of Telemed for Urgent Care
Over the past few weeks, we've been closely watching the impact the novel coronavirus COVID-19...

Solv’s Clinic Analytics magnifies urgent care reporting and insights
Consumer expectations continue to expand, as does the weight of their impact. As a result, the...

5 Secrets to a Happier Urgent Care Staff and More Loyal Patients
A happy staff and more loyal patients are within your reach. You just need the right formula....

Managing an Urgent Care Front Desk and Putting the Patient First
Have you ever seen a disorganized reception area at a clinic? Phones were probably ringing for...

State of American Healthcare: The Staff Experience
This is Part 4 concluding our series on the State of American Healthcare. Don't miss the previous...

Hire the Right People at Your Urgent Care
Your patients and your bottom line matter a lot. So does your team. Your team is comprised of...

Introducing Solv Video Telemedicine
Today we’re excited to announce the launch of Solv’s newest product —Solv Video Telemedicine....

How to Help Your Patients Manage Allergies
Experts are speculating that the 2018 asthma and allergy season may be the worst the U.S. has...

The "Five Rs" of Proper Urgent Care Clinic Maintenance
Are your janitors costing you patients?Urgent Care Centers are providing a good alternative to...

The Importance of Hiring the Right People at Urgent Care
Your patients and your bottom line matter a lot. So does your team. Your team is comprised of...

Should Your Urgent Care Use a Medical Scribe?
Use of a medical scribe is largely determined by the size of your urgent care operation and...

Should Your Urgent Care Stay Open During the Holidays?
Patients view urgent care clinics as lifelines that fill the gap between primary care and the...
Make New Money and Keep the Old: Increase Urgent Care Revenue
Urgent care clinics are expected to grow substantially as more and more Americans get...

Improve Front Desk Efficiency at Urgent Care Clinics
Your patients and bottom line matter a lot, so does your team. They are your most loyal brand...
Featured articles
- Your New Digital Front Door
- Holiday Season Checklist: 4 Ways to Prep Your Urgent Care for the Busy Season Ahead
- 5 Things Urgent Care Can Learn From Starbucks
- Patients First: How NextCare Connects, Retains, and Delights Patients Across 170+ Clinics with Solv
- 6 Text Messages You Should Be Sending Patients [With Templates!]
- 4 Key Ways to Prepare Operations Before Respiratory Season
- 4 Ways to Fight Inflation in Urgent Care
- How To Market Your Urgent Care: Secrets of Urgent Care Marketing Success in 2023
- 3 Keys to Patient Loyalty In Urgent Care
- The Complete Guide to Urgent Care Financial Management
- 6 Things Urgent Care Brands Can Learn From Apple
- How PhysicianOne Urgent Care Grew Profitability By Focusing on Patient Experience









































![6 Text Messages You Should Be Sending Patients [With Templates!]](https://d1kve3ll6vvkpr.cloudfront.net/dir/media/W1siZiIsIjIwMjIvMDkvMTUvMTYvMTUvNDMvZWVjMWI3ZjYtZjNjYy00MTI5LWE5MmYtZjZmNThjOTZjYzI2L2Jsb2cgYmFubmVycyAoMikucG5nIl0sWyJwIiwidGh1bWIiLCIzNjV4MTkwIyJdLFsicCIsImVuY29kZSIsImpwZyIsIi1xdWFsaXR5IDk1Il1d/file.jpg?basename=6+Text+Messages+You+Should+Be+Sending+Patients+%5BWith+Templates%21%5D&sha=50aca008ad78cd8a)