Key Points
- Consumers are increasingly seeking more information and convenience in managing their healthcare, but past technologies have often been confusing and complicated.
- Solv has developed a mobile application that allows consumers to manage their healthcare on their own terms, with over one-third of Solv's direct bookings coming from the app since its launch in October 2019.
- The Solv app has seen significant user engagement, with app users 34% more likely to add their health insurance and 79% more likely to book a visit with an urgent care center than website users.
- Solv's new insurance tracker feature has been successful, with over one-third of users returning to the app to engage with it, proving that consumers engage more when they have access to personalized, digestible information.
- The Solv app also provides a loyalty loop for users, with 97% of consumers rebooking through Solv returning to the same clinic where they were previously seen, indicating that the app makes managing healthcare easier for consumers.
Consumers continue to prove that they’re hungry for more information about their healthcare and want increased and more convenient access to providers. For the past two decades, many healthcare technologies were confusing, complicated, and required too many clunky steps to do tasks that should be simple, such as booking doctor’s visits or understanding their insurance deductible. But because the technology available wasn’t on par with every other industry, consumers didn’t adopt or didn’t engage.
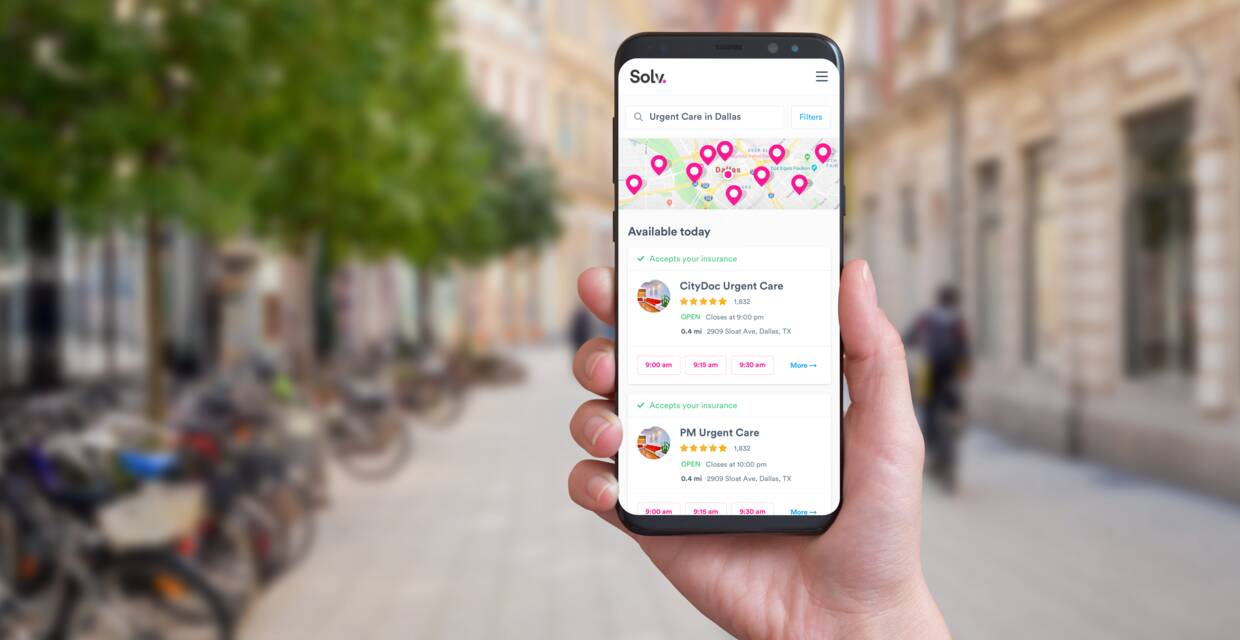
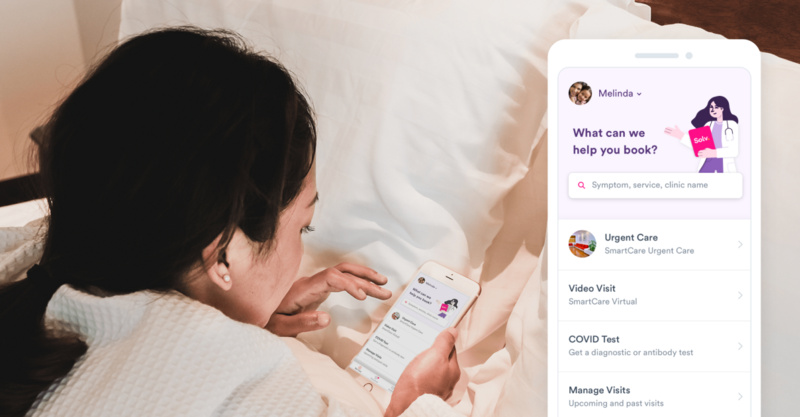
When it comes to managing their healthcare, consumers want to do so on their own terms, no matter where they are. At Solv, we’ve created a way for them to do just that. Since releasing Solv’s first-ever mobile app for iPhone in October, 2019, more than one-third of Solv’s direct bookings have come from the app. Our recent survey found that only 6% of consumers currently manage their healthcare through an app on their phone, but 61% would if it were easy. Between the launch of our iOS app and now the addition of an Android app in the Google Play Store, we’re seeing this confirmed directly by consumer behavior. Solv app users are 34% more likely than website users to add their health insurance and 79% more likely to search for and book a visit with an urgent care center in the app than a Solv user on the website.
Solv is putting even more users in the driver's seat when it comes to their healthcare. With over half a million users opting into Solv’s consumer email messaging in the last year, we’re confident that we’ve cracked the code on providing consumers with the information they need when they need it.

Our newest feature, an insurance tracker that allows users to monitor healthcare spending and access various preventative perks, has proven our hypothesis that empowered consumers with access to personalized, digestible information are more engaged. More than one-third of Solv users are returning to the app to review their insurance and engage with the insurance feature — unprecedented numbers. By giving consumers the data they need in an intuitive way, they can make better informed decisions about where to go for their healthcare and how to effectively use their health insurance to get the best care available to them.
“Consumers want to engage with this information. The Solv iOS and Android apps serve as a new distribution channel for our urgent care partners, giving them an additional touchpoint to engage their patients and drive loyalty,” says Solv’s Head of Product, Gemmy Tsai. The Solv app also provides a loyalty loop for users – 97% of consumers rebooking through Solv return to the same clinic where they were previously seen. “They’re using Solv because it makes managing healthcare easier than ever,” says Tsai.
If you’re a reporter interested in learning more about Solv, email [email protected].
Frequently asked questions
What is Solv and what does it offer to consumers?
Solv is a healthcare technology company that offers a mobile app for consumers to manage their healthcare. This includes booking doctor's visits, understanding insurance deductibles, and monitoring healthcare spending.How have consumers responded to the Solv app?
Since the release of Solv's first-ever mobile app in October 2019, more than one-third of Solv's direct bookings have come from the app. Users are also 34% more likely to add their health insurance and 79% more likely to search for and book a visit with an urgent care center within the app than on the website.What does the Solv app offer that the website does not?
The Solv app offers an insurance tracker feature that allows users to monitor healthcare spending and access various preventative perks. The app also provides a loyalty loop for users, with 97% of consumers rebooking through Solv returning to the same clinic where they were previously seen.What is the current percentage of consumers managing their healthcare through an app?
According to a recent survey by Solv, only 6% of consumers currently manage their healthcare through an app on their phone.What percentage of consumers would manage their healthcare through an app if it were easy?
According to the same survey, 61% of consumers would manage their healthcare through an app on their phone if it were easy.How does Solv engage with its users?
Solv engages with its users by providing them with personalized, digestible information about their healthcare. This includes information about their insurance, healthcare spending, and where to go for their healthcare.How does the Solv app benefit its urgent care partners?
The Solv app serves as a new distribution channel for Solv's urgent care partners, giving them an additional touchpoint to engage their patients and drive loyalty.How can I learn more about Solv?
If you're interested in learning more about Solv, you can email [email protected].